Goal 1
OBJECTIVE
- Promote and support policies, systems and environmental changes that optimize healthy living through good nutrition, increased physical activity and tobacco avoidance
- Promote and support policies, systems and environmental changes to reduce exposure to environmental carcinogens and cancer-related infectious agents
STRATEGIC ACTIONS
- Advance awareness of the types of policy and environments that support cancer preventive nutritional choices, such as daily access to a variety of fruits and vegetables and avoidance of heavily processed foods
- Support policy, systems and environmental changes to create opportunities for physical activity where Connecticut residents live, work, play and learn
- Collaborate with state and local agencies to implement policy for tobacco-free living and the support of cessation efforts
- Promote the use of environmental changes, such as shade structures, to reduce the risks of harmful UV exposure
- Advocate for policies that reduce the risks of harmful UV exposure through artificial sources
- Advocate for evidence-based interventions to reduce exposure to and infection with cancer-related infectious agents (such as HPV, hepatitis B and C and HIV)
- Monitor trends in data related to cancer risk, including trends in relative cancer risk among priority populations
Why This is Important
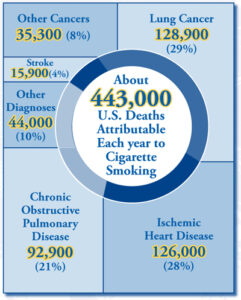
- The U.S. Centers for Disease Control and Prevention (CDC) recommends that Connecticut spend $43.9 million a year to have an effective, comprehensive tobacco prevention program. Connecticut currently allocates $6.0 million a year for tobacco prevention and cessation. This is 13.7 percent of the CDC’s recommendation and ranks Connecticut 23rd among the states in the funding of tobacco prevention programs. Connecticut’s spending on tobacco prevention amounts to 1.1 percent of the estimated $535 million in tobacco-generated revenue the state collects each year from settlement payments and tobacco taxes. (36) Smoking is known to cause cancers of the lung, esophagus, larynx, mouth, throat, kidney, bladder, pancreas, stomach and cervix, as well as acute myeloid leukemia.
- In Connecticut, rates of tobacco use are associated with income and education. Among persons earning less than $15,000 per year, tobacco use is substantially higher than those earning $50,000 or more, 26.6 percent versus 10.7 percent.
- Overweight and obesity are clearly associated with an increased risk for developing many types of cancer. About one-quarter to one-third of new cancer cases in the U.S. in 2013 will be related to overweight or obesity, physical inactivity and poor nutrition. Fewer opportunities for physical activity and less access to fresh fruits and vegetables generally adversely affect persons with low socioeconomic status. Policy, systems and environmental changes can help to alleviate these health inequities.
- Among students in grades 9-12 in the 2011 Connecticut Youth Risk Behavior Survey 20 percent of females and 33 percent of males were overweight and/or obese. Rates were significantly higher among black (43.9 percent) than white (21.1 percent) students. (38)
- Connecticut has one of the highest skin cancer incidence rates in the country. (39, 40) The rate of new melanoma diagnoses—responsible for 75 percent of all skin cancer deaths—was 24 percent higher in Connecticut than the national average from 2006-2010 and was the 11th highest in the U.S. An estimated 934 state residents were diagnosed with melanoma in 2010. The recent ban on indoor tanning for minors under the age of 17 is an example of a policy change as an effective and far-reaching course of action.
- Populations that include large numbers of recent immigrants, such as Hispanics and Asians, have higher rates of cancer related to infectious agents. Hispanic women have the highest incidence rate for cervical cancer. The U.S. Food and Drug Administration has approved two types of vaccines to prevent cancer: vaccines against the hepatitis B virus, which can cause liver cancer, and vaccines against human papillomavirus (HPV) types 16 and 18, which are responsible for about 70 percent of cervical cancer cases. The HPV vaccine is recommended for females aged nine to 26 and males aged nine to 21. It protects against the HPV types that most often cause cervical, vaginal, vulvar, and anal cancers. Additionally, studies show that about 60 to 70 percent of cancers of the oropharynx may be linked to HPV.
- Connecticut blacks and Hispanics are disproportionately impacted by HIV and thus bear increased added burden of HIV associated cancer risk. Early and sustained antiretroviral therapy for persons with HIV is a crucial cancer prevention strategy
PROMISING PRACTICES
- The Community Transformation Grant (being implemented by five Connecticut counties) has identified tobacco-free living as one of three strategic directions. Focused on policy implementation at the local level, these communities are looking to establish tobacco-free parks and other public spaces (including multi-unit housing
- Healthy Restaurant designation is an initiative in ACHIEVE communities to promote healthy living. It aims to encourage restaurant owners to provide healthy options. The model focuses on always having a fresh non-cooked, non-processed fruit or vegetable available as a side dish or addition and having American Heart Association-recommended portions available.
- The National Prevention Strategy of the National Prevention, Health Promotion and Public Health Council has developed a comprehensive plan to improve the health of the nation with investments in prevention and public health programs.
